Can Anxiety Cause High Blood Pressure? A Physician Explains
If a patient asked me, “Is it too hot in Omaha, Nebraska?” I couldn’t answer without more information. Is it morning or noon, winter or summer? Context changes the answer.
The same principle applies to blood pressure. Like the weather, blood pressure is always on the move, rising and falling throughout the day. A single number, taken out of context, can be as misleading as a cholesterol reading without a calcium score.
If this concept, that context dictates the answer, is the only information you take away from this blog post, the read was worth your time.
Can Anxiety Cause High Blood Pressure?
Yes, anxiety can cause high blood pressure temporarily. When we feel stressed, our bodies translate the emotional experience into biology through hormones like adrenaline and cortisol. These hormones increase heart rate, constrict blood vessels, and increase blood flow throughout the body.
The result: blood pressure goes up. Chronic stress can even change the way our bodies store and distribute fat, compounding the cardiovascular burden over time. Whether that spike is harmful depends, once again, on context.
We evolved this hormonal surge, called the sympathetic response, to give us power when we need it. Our ancestors needed that rush of adrenaline to escape a saber-toothed tiger. The response is adaptive; it kept our species alive.
The distinction is duration. If the spike is temporary, it’s adaptive. If stress and high blood pressure become chronic, it’s no longer protective; it’s a disease called hypertension, and it damages blood vessels, the heart, and organs over time.
White Coat Hypertension: The Modern Saber-Toothed Tiger
We’ve all lived this scenario: You left for the doctor’s office late. Traffic was worse than expected. The parking lot was full. The office was on the second floor, and you couldn’t wait for the elevator. You ran up, sat down, and the medical assistant immediately strapped the blood pressure cuff on you.
Under these conditions, the modern equivalent of the saber-toothed tiger has your hormones firing. I’ve experienced this situation myself. I’ve seen my own blood pressure read 150/100 in the office when, on a restful day at home, I’m closer to 120/70. (I’ve written about my high blood pressure experience in more detail on our blog.)
This phenomenon is called “white coat hypertension.” A white coat is what physicians traditionally wore in medical settings. If you know what a phone booth is, you probably remember the white coat, too. And if you remember the little plastic adapter for 45 RPM records, it’s time for a colonoscopy.
White coat hypertension affects 15–30% of people who get blood pressure readings in a doctor’s office. Even without rushing to get there, the environment itself can trigger enough cortisol and adrenaline to produce an artificially elevated reading.
How to Get an Accurate Blood Pressure Reading
If anxiety and blood pressure readings are so closely tied to context, the next logical question is: what are the correct conditions for an accurate reading?
The American Heart Association guidelines are specific.
Before the reading: Sit quietly for three to five minutes without talking or moving. For the prior 30 minutes, avoid caffeine (and know how long caffeine stays active in your system), exercise, and smoking. Empty your bladder.
Your positioning: Keep your feet flat on the floor, not dangling from an exam table. Rest your back against a chair. Place your arm on a desk or table at the level of the heart. That last point deserves special attention, and you can test it on yourself right now.
At the top of your sternum (the bone in the center of your chest), you’ll feel a small V-shaped notch called the sternal notch. At the very bottom of that bone, before it gives way to your abdomen, you’ll find a small point called the xiphoid process.
Halfway between those two landmarks is where your heart sits. The blood pressure cuff on your arm needs to be at that height.
If the cuff sits below the level of your heart, the reading will be falsely elevated. I can’t overstate how often I see this done incorrectly.
One more detail: Your arm must be passively supported at that height. Using muscle tension to hold your arm up changes how the artery runs through the bicep and skews the reading.
During the reading: The cuff needs to be the correct size. Place it on bare skin, not over clothing. Remain silent and relaxed. Deep breathing helps. Take multiple readings, spaced a few minutes apart, and average them.
Following all these rules is nearly impossible during a typical doctor’s office visit. Getting an accurate picture of your blood pressure requires monitoring at home.
Modern home blood pressure cuffs are fairly accurate. Try different times of day, follow the rules above, and bring the results to your next appointment.
Can Repeated Anxiety Spikes Lead to Chronic Hypertension?
Yes. The medical literature shows an association between frequent anxiety-driven spikes and the development of chronic hypertension.
The more nuanced question is causality. Are the spikes themselves causing chronic high blood pressure? Or does anxiety, more broadly, skew your hormonal balance over time, and that hormonal imbalance is what drives hypertension?
It’s a distinction without a difference. Anxiety management tools are blood pressure management tools. Addressing anxiety, whether through breathing techniques like belly breathing, exercise, sleep, or other stress-reduction practices, directly supports cardiovascular health.
True Hypertension vs. a High Blood Pressure Reading
A single elevated reading in the doctor’s office doesn’t mean you have hypertension. True hypertension is what you discover when you follow all the rules at home, take readings at different times of day, average the results, and still see elevated numbers consistently.
The medical community categorizes blood pressure into stages: normal, elevated, stage 1 hypertension, and stage 2 hypertension. Each stage has specific numerical cutoffs that guide treatment decisions. For a detailed breakdown of those stages, refer to our post on how long blood pressure medicine takes to reach its full effect.
If your home readings confirm pre-hypertension or hypertension, that’s the starting point for a conversation with your physician about management.
Managing Anxiety and High Blood Pressure
For mild elevations without additional risk factors, your physician will likely start with lifestyle modifications:
- More sleep
- Regular exercise (even walking 10,000 steps a day can make a measurable difference)
- Weight management
- Reduced alcohol intake
- Stress reduction (wearable devices that track heart rate variability can help you monitor stress levels and measure your progress)
If lifestyle changes don’t bring your numbers into range, or if your blood pressure is higher and you have additional risk factors, you’ll enter a discussion with your physician about medication. The prescription for managing high blood pressure is always lifestyle plus or minus medication.
You won’t be told to skip the lifestyle changes and rely on pills alone. Pharmacologic treatment builds on maximizing every non-drug intervention first.
Today’s Takeaways
Anxiety can cause high blood pressure temporarily, and over time, chronic anxiety may contribute to true hypertension.
Invest in a high-quality home blood pressure cuff and learn the rules for accurate measurement. Next time you get your blood pressure checked in a healthcare setting, advocate for proper technique. The staff taking your reading may not have the time or awareness to follow every guideline, but now you do.
At Banner Peak Health, we spend time helping our patients distinguish between a stress-driven spike and a true pattern of hypertension. That distinction, and the personalized management plan that follows, is the kind of care we believe every patient deserves.

5 Weird Signs of Iron Deficiency Your Doctor Might Not Mention
Most people equate iron deficiency with anemia: feeling tired, looking pale, and running low on energy. That picture isn’t wrong, but it’s incomplete.
Anemia means your blood doesn’t carry enough hemoglobin, the protein in red blood cells that delivers oxygen from your lungs to the rest of your body. About 60% of your body’s iron lives in hemoglobin, which is why routine bloodwork and lab testing focus on red blood cell counts. The other 40% does work that most patients never hear about.
Iron deficiency symptoms affect virtually every system in your body. Iron fuels the enzymes in your mitochondria (your cells’ energy producers), helps your brain manufacture neurotransmitters, builds myoglobin (a local oxygen reserve inside muscle cells), drives DNA synthesis and repair, and supports immune cell function.

When iron runs low, the consequences don’t stop at fatigue. Hair loss, brittle nails, and exercise intolerance are common. The five weird signs of iron deficiency below are ones my patients never see coming.
5 Weird Signs of Iron Deficiency Your Doctor Might Not Mention
1. Restless Leg Syndrome
About 30% to 40% of people with low iron develop restless leg syndrome, an uncomfortable and persistent urge to move the legs, especially at rest and at night. The sensation can range from a tingling to an aching that only subsides with movement, and it can be severely disruptive to sleep quality.
The mechanism happens at the brain level. Without adequate iron, your brain can’t produce enough dopamine, and this reduced dopamine production triggers restless leg syndrome. Even when blood iron levels are only mildly low, the brain can experience a severe deficit, making neurological symptoms appear long before anemia shows up on standard labs.
2. Compulsive Ice Cravings
Pagophagia, the medical term for compulsive ice chewing, occurs in 40% to 50% of iron-deficient individuals. Patients describe an intense, almost addictive need to chew ice, sometimes consuming bags per day. The craving disappears when iron levels return to normal.
The physiology behind this is one of the most fascinating iron deficiency symptoms I’ve encountered. Chewing ice lowers the temperature in your mouth, which reflexively dilates blood vessels in your brain and increases blood flow to compensate for impaired neurotransmitter production. Studies confirm that iron-deficient individuals experience measurable cognitive improvement from ice chewing, an effect absent in people with normal iron levels.
This reflex explains a familiar phenomenon: ice cream headaches. Brain freeze causes the same blood vessel dilation mechanism, but in a person who doesn’t need the extra blood flow to the brain.
The dilation becomes painful instead of therapeutic. It’s two sides of the same coin.
3. Spoon-Shaped Nails
Koilonychia, or spoon-shaped nails, is one of the more visually distinctive low-iron signs. The nails curve upward at the edges, forming a concave shape, almost like a tiny spoon.
Nail bed cells divide rapidly and need functioning DNA synthesis and cell repair pathways to manufacture the nail plate correctly. When iron stores drop, the manufacturing process breaks down, and the nail develops an abnormal shape.
Any cell in the body that turns over quickly, including nail, hair, and skin cells, depends on adequate iron to maintain normal growth.
4. Painful Tongue and Cracked Mouth Corners
A swollen, red, painful tongue (atrophic glossitis) and cracks at the corners of the mouth (angular cheilitis) are among the lesser-known signs of iron deficiency. These symptoms send patients to dentists and dermatologists who may treat the surface-level problem without investigating the underlying cause.
The mechanism is the same rapid cell turnover issue that affects nails: The cells lining your mouth and tongue divide constantly and depend on iron for normal DNA function. When the body depletes its iron stores, those tissues can’t repair and regenerate properly. A thorough annual physical exam that includes ferritin testing can connect these oral symptoms to their true source.
5. Cognitive and Emotional Changes
Of all the weird signs of iron deficiency, this one is the most underdiagnosed and potentially the most damaging. Concentration problems, poor attention, irritability, depression, and heightened stress responses can all stem from inadequate iron.
Iron is necessary for synthesizing dopamine, serotonin, and norepinephrine, three neurotransmitters that regulate nearly every aspect of brain processing. Low iron disrupts the production of these chemical messengers, and the cognitive and emotional symptoms can mimic or overlap with early signs of dementia and mood disorders. These iron deficiency symptoms often reverse with proper treatment, making this one of the most correctable causes of cognitive decline I encounter in practice.
Why Standard Blood Tests Miss Iron Deficiency
Iron deficiency progresses in stages, and standard blood panels only catch the final one.
A complete blood count (CBC) measures hemoglobin, red blood cell size, and red blood cell count. These values don’t drop until iron depletion has advanced to full-blown anemia. By that point, the body has been running on empty for months.
Your CBC is your checking account, the money you spend day to day. Ferritin is your savings account. Your body will drain the savings (ferritin) to keep the checking account (CBC) operational, but the depleted savings still affect your health long before the checking account runs dry. To catch iron deficiency symptoms early, you need a ferritin level drawn alongside your standard metabolic panel.
Ferritin below 30 indicates iron deficiency in otherwise healthy individuals. Some studies suggest patients feel better with levels above 50. If you’re experiencing any of the symptoms above, ask for ferritin testing by name.
What Causes Low Iron Levels
The first step in treating iron deficiency is identifying the root cause. The answer falls into two categories: too little iron getting in, or too much iron going out.
Iron is widely available in the diet from both animal and plant sources, so inadequate intake is rarely the primary culprit (with some exceptions for vegans and vegetarians, who face a slightly higher risk from the lower bioavailability of plant-based iron). The bigger factors are absorption problems and ongoing losses.
Approximately 38% of reproductive-age women have iron deficiency, even without anemia. Menstruation and pregnancy both draw heavily on iron stores. Low-level GI bleeding from ulcers or polyps is another common source of loss.
One of the most overlooked causes of low iron levels in modern medicine is impaired absorption due to acid-suppressing medications. Millions of people take proton pump inhibitors (brand names like Prilosec and Protonix) and H2 blockers (like Pepcid) for GERD and gastritis. The body needs an acidic stomach to absorb iron from food, and these drugs reduce that acidity.
If you’re taking acid-suppressing medications and noticing any of the symptoms above, discuss GI health and supplementation with your physician.
Today’s Takeaways
Low iron manifests in ways most people would never anticipate. Restless legs, compulsive ice chewing, misshapen nails, oral tissue breakdown, and cognitive decline are all the five weirdest signs of iron deficiency standard blood tests can miss.
The cognitive and emotional impact of iron deficiency may be the most consequential and the most treatable. Anyone experiencing unexplained concentration problems, mood changes, or persistent fatigue deserves a ferritin test alongside a CBC. This is one of the most prevalent and most correctable causes of symptoms that patients and physicians alike tend to overlook.
At Banner Peak Health, we’re incorporating ferritin testing more broadly into our routine screening. If any of these signs of iron deficiency sound familiar, contact us to schedule a visit. A single blood draw can provide answers that change how you feel and function every day.
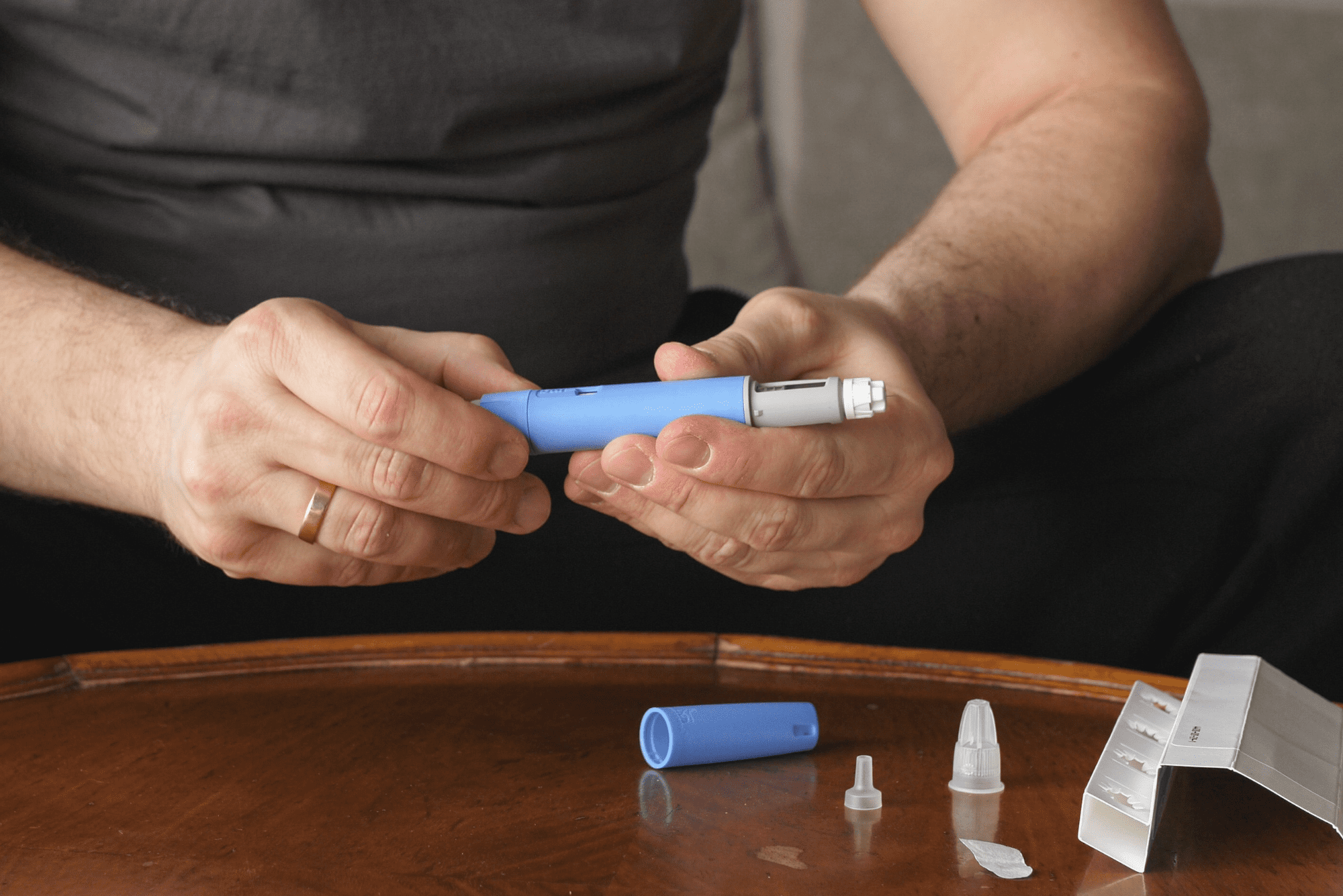
Tirzepatide vs. Semaglutide: A Doctor Breaks Down the Differences
To quote a bumper sticker, if you’re not confused, you’re not paying attention.
I say this often to patients who walk into my office asking about weight loss medications. The differences between tirzepatide and semaglutide are buried under overlapping brand names, competing advertisements, and social media noise. I’ve written about GLP-1 agonist side effects and cautions, and the most common request I receive now is a clear comparison.
The tirzepatide vs. semaglutide matchup isn’t as close as the marketing suggests. The data points in one direction, with cost and convenience as the only real counterweights.
Tirzepatide vs. Semaglutide: Brand Names
Before comparing tirzepatide vs. semaglutide, we need to untangle the naming confusion. I’m a physician, and I had to double-check this myself.
The same drug can carry different brand names depending on whether it’s prescribed for type 2 diabetes and A1C reduction or for weight management.
| Drug | Brand Name | Manufacturer | Approved Use | Form |
| Tirzepatide | Mounjaro | Eli Lilly | Type 2 Diabetes | Weekly injection |
| Tirzepatide | Zepbound | Eli Lilly | Weight Management | Weekly injection |
| Semaglutide | Ozempic | Novo Nordisk | Type 2 Diabetes | Weekly injection |
| Semaglutide | Wegovy | Novo Nordisk | Weight Management | Weekly injection |
| Semaglutide | Rybelsus | Novo Nordisk | Type 2 Diabetes | Daily oral tablet |
Mounjaro and Zepbound are the same drug (tirzepatide), made by Eli Lilly. Ozempic, Wegovy, and Rybelsus are all semaglutide, made by Novo Nordisk. Rybelsus is the only oral formulation available in either drug class.
How Tirzepatide and Semaglutide Work Differently
Our bodies aren’t simple if/then machines. They’re complex webs of hormones, receptors, and feedback loops. When we bring that perspective to the differences between tirzepatide and semaglutide, the mechanism becomes clearer.
Semaglutide activates one hormone receptor: GLP-1 (glucagon-like peptide-1). The lower intestine releases GLP-1 after eating. It stimulates insulin release when blood sugar rises, slows food’s transit through the digestive tract, reduces appetite through direct effects on the brain, and suppresses glucagon (a hormone that raises blood sugar).
Tirzepatide activates two hormone receptors: GLP-1 and GIP (glucose-dependent insulinotropic polypeptide). The upper intestine releases GIP in response to eating. GIP stimulates insulin release when blood sugar rises and influences how the body stores and uses energy.
That dual action touches on the same metabolic tug-of-war between building and breaking down tissue that governs how we gain or lose weight.
If one drug moves one lever and the other moves two levers, the two-lever drug will have a greater impact on the machine. The outcome data confirms this across nearly every measure.
Tirzepatide vs. Semaglutide for Weight Loss
The head-to-head data comes from the SURMOUNT-5 study, one of the longest trials directly comparing these two medications. The study enrolled patients with obesity (without diabetes) and followed them for 72 weeks.
Tirzepatide produced 20.2% weight loss compared to 13.7% with semaglutide, a 6.5-percentage-point gap. In actual pounds, patients on tirzepatide lost an average of 50 pounds, compared with 33 pounds with semaglutide.
Real-world data supports these findings. A study tracking 18,000 patients over 12 months confirmed tirzepatide patients lost 15.3% of their body weight, compared to 8.3% with semaglutide.
For anyone evaluating tirzepatide vs. semaglutide for weight loss, it’s important to explore what’s happening to body composition beyond BMI underneath those results.
Tirzepatide vs. Semaglutide for Blood Sugar and Heart Health
Weight loss is one piece of the picture. For patients managing type 2 diabetes, glycemic control and cardiovascular protection matter just as much.
The SURPASS-2 trial compared tirzepatide and semaglutide for blood sugar management. Tirzepatide at 15 milligrams reduced hemoglobin A1C by 2.3 percentage points, compared to 1.86 percentage points with semaglutide at one milligram.
More striking, 46% of tirzepatide patients reached near-normal blood sugar levels (A1C below 5.7%), versus only 19% on semaglutide. For patients already monitoring their glucose levels, that gap can mean the difference between medication dependence and metabolic freedom.
For cardiovascular health, the two medications offer comparable protection against heart attack, stroke, and cardiovascular death. Tirzepatide shows a slight edge in blood pressure reduction and cholesterol improvement, with HDL increasing by 7%–8% versus 4% with semaglutide. If you’ve been keeping an eye on your non-HDL cholesterol levels, those incremental gains can compound over time.
Across metabolic outcomes, the comparison between tirzepatide and semaglutide ends either in a tie or a tirzepatide advantage.
Tirzepatide vs. Semaglutide Side Effects
Both medications carry a high rate of gastrointestinal side effects: nausea, diarrhea, vomiting, and constipation. These symptoms are usually mild, and patients can manage them by gradually increasing the dosage over several weeks.
Tirzepatide, the more potent of the two, actually carries a lower incidence of GI side effects. In the SURMOUNT-5 study, only 2.7% of tirzepatide patients stopped treatment due to GI symptoms. Twice as many semaglutide patients had to discontinue for the same reason.
A separate concern applies to both medications: lean body mass loss. When the number on the scale drops, some of that loss comes from muscle and bone, not fat. Studies on GLP-1 agonists have shown that up to 39% of total weight loss can come from lean mass, a ratio worse than that of older weight-loss drugs.
Preserving muscle and bone matters more as we age, which is why pairing either medication with a resistance-training program is the best countermeasure I know of.
Today’s Takeaways
When a patient asks me about tirzepatide vs. semaglutide, the conversation is usually short. For weight loss, blood sugar control, cardiovascular markers, and tolerability, tirzepatide is the better drug across all measures. The data from SURMOUNT-5 and SURPASS-2 aren’t ambiguous.
Two factors can shift the calculus. The first is cost: Tirzepatide is more expensive, and insurance coverage varies. If financial access is a barrier, semaglutide remains an effective option with strong clinical evidence behind it.
The second is convenience. Semaglutide is the only one of these two drugs available as an oral tablet (Rybelsus). For patients who can’t tolerate injections, whether from needle aversion, localized skin reactions, or travel logistics that make managing metabolic health on the go more complicated, the oral route matters.
At Banner Peak Health, we evaluate every patient’s full clinical picture before recommending either medication. The right drug depends on your health goals, your metabolic profile, and your practical circumstances.
If you’re considering either option, contact us to schedule a visit. We’re happy to walk through the data together.
The Link Between Melatonin and Heart Failure: A Doctor Reviews the Evidence
When I don’t like my wife’s outfit and she asks for my opinion, I tell her.
People are often surprised I’d say that, but honesty gives my approval meaning. We’ve been together over 30 years, so it must be working.
The same principle applies in medicine. How often do you hear a physician say, “I don’t know”? Given how fast medical knowledge expands, what any doctor doesn’t know vastly exceeds what they do. Failing to admit that undermines faith in all their other claims.
At Banner Peak Health, we embrace the “I don’t know.” That intellectual humility creates the passion to find answers. The tool we reach for is Open Evidence, a medical AI platform built exclusively on published clinical literature, launched in 2023.
Unlike general AI, it doesn’t hallucinate. We use it daily, often hourly. I’ve previously written about how melatonin affects your sleep cycle, but when a patient recently asked about the link between melatonin and heart failure, my honest answer was, “I have no idea.”
So I opened Open Evidence, and what I found in a few minutes blew me away.
What Open Evidence Taught Me About Melatonin and Heart Failure
Melatonin usage is not a risk factor for heart failure. A large study tracked a patient population for 23 years and found no association between regular melatonin use and cardiovascular disease of any kind, including congestive heart failure.
What surprised me was the next finding. A growing body of evidence links taking melatonin to potential benefit for people already living with congestive heart failure.
A randomized, double-blind, placebo-controlled trial enrolled 92 patients with heart failure from reduced ejection fraction. Patients received 10 milligrams of melatonin daily for 24 weeks and showed measurable improvement across several physiological parameters.
A meta-analysis of three studies on melatonin as a treatment confirmed improvements in quality of life, reduced fatigue, better sleep, and improved cardiac markers, including pump function. Melatonin, the supplement millions take to fall asleep, shows measurable improvements in heart performance. That’s not what I expected to find.
Why Researchers Connected Melatonin and Heart Failure
The next question Open Evidence helped me answer: Where did this idea even come from?
Three lines of evidence converge. People with chronic heart disease, including coronary artery disease and congestive heart failure, tend to have lower plasma melatonin levels. That association raised a hypothesis: If you raise melatonin exogenously, maybe you can improve cardiac function.
Animal models added two more pathways. Melatonin has direct antioxidant activity, reducing reactive oxygen species that drive degenerative disease, and it supports better mitochondrial function and cellular energy production. Researchers have identified melatonin receptors in heart tissue, suggesting a physiological link between melatonin and cardiac function.
That’s why controlled trials started.
Why This Isn’t Ready for Clinical Practice
The evidence is intriguing, but it isn’t sufficient.
The longest trial here ran 24 weeks. Congestive heart failure is a lifelong condition, and proof of concept over 24 weeks isn’t enough to change how we practice. The dose used in these studies, 10 milligrams, is at least 10 times what’s needed for sleep, making it supraphysiologic by any measure.
Over-the-counter melatonin preparations rarely disclose content or purity reliably. How you choose supplements matters, especially at doses this high. High-dose melatonin may worsen insulin resistance, which likely explains why the cardiac improvements in these studies appeared only in non-diabetic patients.
Today’s Takeaways
The melatonin and heart failure story is a good example of what intellectual humility looks like in practice. I didn’t know the connection existed. I used the right tool to find out, and I came away with a nuanced answer: Melatonin doesn’t cause heart failure, the early signals for benefit are real, and the evidence isn’t yet strong enough to act on clinically.
That “not yet” is as meaningful as the finding itself. At Banner Peak Health, that commitment to evidence-based preventive care shapes every conversation we have with patients. The first step in learning is being willing to say you don’t know.

The Science Behind How to Regulate Body Temperature at Night
Who doesn’t love freshly baked bread?
Bread, like sleep, is a time-ordered process that depends on having the right temperature at the right time. First, we need time to let the dough rise in a warm environment, allowing the yeast to do its work. Then, when it’s time to bake the loaf, we need the higher temperature of the oven for the chemical reactions to occur. Finally, when the bread is finished, a distinct cooling process lets the final structure set before it’s ready to eat.
Sleep is a temperature-dependent process, too. Learning how to regulate body temperature while sleeping starts with understanding this cycle.
Our body temperature fluctuates over 24 hours, peaking between 6 and 8 p.m. To fall asleep in the evening, a cooling process must occur. We reach our nadir, or low point, between 4 and 6 a.m., after which our body temperature rises to help us wake.
And like bread, when the process doesn’t go well, it results in crumby sleep. (Please laugh.)
How Temperature Affects Sleep: The Brain Connection
The preoptic area of the hypothalamus is the region of the brain that regulates both sleep and body temperature. It integrates these two processes because they’re interconnected. Body temperature is inextricably linked to sleep.
Understanding how temperature affects sleep requires understanding how we regulate our temperature in the first place.
Core Temperature vs. Peripheral Temperature
We have two locations of body temperature to consider:
- Core body temperature is what you’d measure with a thermometer under your mouth (or rectally, for infants)
- Peripheral body temperature is what a wearable like an Oura Ring measures at your fingertips or extremities
Our body uses different tools to regulate core body temperature. To raise core temperature, we can:
- Enhance metabolism (shivering, burning more calories)
- Reduce blood flow to the periphery through vasoconstriction
To lower core temperature, we can:
- Slow down metabolism
- Increase blood flow to the periphery through vasodilation
- Sweat
Blood doesn’t just carry oxygen and nutrients. It also carries heat energy. Our periphery has many blood vessels on its surface, which act like radiators. The more blood that flows to the periphery, the more heat energy is lost from the body.
When we vasoconstrict, those small arteries tighten, reducing blood flow to the surface and conserving heat in the core. When we vasodilate, we open those “radiators” and release heat, lowering core body temperature.

Why Hot Environments Disrupt Body Temperature While Sleeping
Most of us have experienced how sleep environment impacts sleep quality. If you’ve ever tried to sleep during a heat wave without air conditioning, you know it’s miserable.
Our body temperature peaks in the early evening. To fall asleep, we need to lower our core body temperature. That can’t happen if the external environment is too warm. Exogenous heat becomes the enemy of healthy body temperature while sleeping.
How to Regulate Body Temperature While Sleeping: Low-Tech Solutions
If external heat can hurt sleep, temperature modulation can enhance it. Some methods to regulate body temperature at night have been around for generations.
The Warm Bath Paradox
We’ve established that exogenous heat impairs sleep, yet taking a warm bath one to two hours before bed, for as little as 10 minutes, has been documented to improve sleep onset and quality.
When you’re in a hot bath, your body absorbs heat energy and responds by vasodilating to dissipate it. When you get out of the bath, you’re still vasodilated. You’ve opened those radiators.
You actually lose more body heat after the bath because of this vasodilation, which lowers your core body temperature and primes your body for sleep.
Warm Socks at Bedtime
The same principle applies to putting on warm socks before bed. This old wives’ tale has a physiological basis: warming your extremities causes vasodilation, which helps dissipate heat from your core.
It’s a simple way to regulate body temperature at night without any special equipment.
How to Regulate Body Temperature at Night: New Technology
On one hand, we have wool socks and warm baths. On the other, we have high-tech solutions like temperature-regulating mattresses.
The leading technology in this space is the Eight Sleep mattress cover, which uses water-filled coils and a pump to adjust the temperature from about 55 to 110 degrees Fahrenheit. The Eight Sleep also uses sensors to detect respiratory rate, heart rate, and temperature to infer what phase of the sleep cycle you’re in, allegedly adjusting temperature accordingly.
Does it work? Two questions are built into this:
- Is modifying external body temperature via a temperature-adjusted mattress effective?
- Can the device accurately identify your sleep phase to deliver the right temperature at the right time?
I dove into the literature, and both questions remain unanswered. The company hasn’t described its sensing technology or validated its accuracy.
One industry-sponsored study exists, but it had only 54 subjects with a mean age of 36. Younger people sleep more easily, making this an unchallenging test population. The methodology involved only eight nights (four with, four without), and while it showed some improvement, the overall study design was too weak to draw conclusions.
The device costs $3,000–4,000. It offers a 30-day money-back guarantee. Like many new technologies, it’s commercially available and holds high promise, but we lack solid evidence of its efficacy.
How Temperature Affects Sleep: Individual Variability
How temperature affects sleep varies across individuals, genders, pre- and post-menopause, and age groups. You need to be attuned to what works for you. My ideal 64 degrees might be your ideal 71 degrees.
For couples, this creates a common challenge. More often than not, partners can’t come to a consensus on sleep temperature.
Be prepared to defend your individual needs. Anyone who’s shared a bed knows this struggle.
Bedding and Sleepwear
What about pajamas and bed covers? The gurus speak as if natural fibers and breathability are gospel, but no scientific studies definitively prove this.
That said, based on first principles, it makes sense. Your body needs to modulate temperature throughout the night, sometimes releasing heat, sometimes conserving it. Natural fibers that breathe and don’t trap heat allow your body to self-regulate better than synthetics.
The evidence isn’t there, but the logic is sound. Choosing breathable fabrics is one more way to regulate body temperature while sleeping.
How to Regulate Body Temperature While Sleeping: Today’s Takeaways
Understanding how to regulate body temperature while sleeping comes down to a few key principles:
- The temperature of your environment is intimately linked to your ability to sleep. This isn’t theory. It’s biology, controlled by the same part of your brain.
- Tried-and-true low-tech solutions work. A warm bath one to two hours before bed, warm socks, and a thermostat set to your personal comfort level are all validated approaches for managing body temperature while sleeping.
- Respect individual variability. Don’t chase a specific number. Experiment to find what works for you, and in shared sleeping arrangements, advocate for your needs.
- New technology shows promise but lacks proof. Products like the Eight Sleep mattress are commercially available, but the science hasn’t caught up to the marketing.
At Banner Peak Health, we’re fascinated by sleep and watching this space closely. Stay tuned for further developments.
The Truth About How to “Reset Your Metabolism” (And What Actually Works)
The other night, our new induction stove displayed an error message. The screen flashed a code I didn’t recognize, so I did what any person living in the 21st century would do: I consulted ChatGPT.
The answer was simple: Reset the stove by flipping the circuit breaker off and back on. No forward-facing power switch existed, so I bundled up, trudged outside in the cold, found the breaker box, and flipped the switch.
After a moment, I flipped it back on. The error vanished. Problem solved.
Walking back inside, I thought, “Wouldn’t it be wonderful if we could do the same thing with our bodies? Especially our metabolic health?”
If something feels off (weight creeping up, energy crashing, blood sugar spiking), we want to flip a switch and return to factory settings. This instinct makes perfect sense. We’re 21st-century humans surrounded by technology, and “reset” is our default problem-solving approach.
But our bodies don’t work that way.
If you’ve ever searched “how to reset your metabolism,” you’re not alone. Grasping why that search leads nowhere is the first step toward real metabolic health.
What “Reset Your Metabolism” Really Means
The phrase “how to reset your metabolism” gets searched thousands of times each month. Patients come to me asking for the metabolic equivalent of that circuit breaker: some pill, supplement, or cleanse that will flip everything back to optimal.
Metabolism, like all our health systems, is dynamic. It doesn’t sit at a fixed point waiting to be “reset.” It’s more like a sailboat than a stove. Wind pushes against the sails. Waves rock the hull. Currents pull in unexpected directions.
The boat stays upright not because it’s frozen in place, but because it constantly adjusts, leaning into the wind, correcting course, and rebalancing against every force trying to knock it over.
That’s your metabolism.

Source: Canva
The Science of Staying Upright: Homeostasis
The medical term for this continuous rebalancing is homeostasis. It’s the most important concept for grasping health and aging.
Think about everything that tries to knock you off course: illness, sleep deprivation, injury, dehydration, stress, etc. We need the resiliency to keep correcting and maintaining equilibrium, no matter what life throws our way.
When you think of the word “reset,” you imagine a single moment: returning to one correct position one time. But health isn’t reaching a destination. It’s your ability to get to that destination again and again.
Why You Can’t Reset Your Metabolism With Pills and Supplements
A pill or supplement doesn’t address the core route to health. It just reduces the danger of your body being out of balance.
Take high blood pressure. If your body isn’t maintaining homeostatic balance, your blood pressure rises. That elevation increases your risk of stroke, heart attack, and kidney damage.
We prescribe medication to bring that number down. But the medication doesn’t rebalance your body. It makes being out of balance less dangerous.
The same applies to blood sugar medications, cholesterol drugs, and supplements marketed to reset your metabolism. They may reduce risk, but they don’t restore the ability to self-regulate.
That pill doesn’t get you off the hook for your own lifestyle choices. A physician can prescribe medication, advise you, and point you in the right direction, but the ultimate responsibility for your health rests with you and the choices you make.
You can’t outsource your health to a doctor or supplement. You own it.
The Real Pillars of Metabolic Health
If we abandon the reset mindset in favor of a support mindset, what does that look like in practice?
The foundational pillars are familiar but bear repeating: nutrition, movement, sleep, and stress management. These aren’t sexy, but they influence your body’s ability to maintain equilibrium.
All of life, we are that sailboat, being pushed by winds and rocked by waves. As we age, we don’t right ourselves as quickly. We spend more time leaning, more time off-balance. That’s the disease state. Eventually, if we can’t right ourselves at all, we capsize.
The goal isn’t to never get knocked off course. We need to build the resilience to recover, again and again.
The Danger of Diets That Promise to Reset Your Metabolism
Popular diets and detoxes make bold promises. From a clinical perspective, these extreme approaches often do the opposite of what they claim.
Consider the logic through the lens of homeostasis. If balance is the goal, what happens when you drastically hurl yourself away from the center?
You don’t strengthen your long-term equilibrium. You destabilize it further. Trendy diets don’t address your body’s ability to self-regulate. They just yank the sailboat in the opposite direction temporarily.
When you stumble upon a new health intervention, ask yourself, “Does this support my body’s ability to maintain balance over time? Or does it just promise dramatic short-term change?”
Today’s Takeaways
You can’t reset your metabolism with a pill, cleanse, or crash diet, because metabolic health is about building your body’s capacity to right itself against whatever forces try to knock it down.
Start with one sustainable change. Maybe it’s consistent sleep timing, a daily walk, or reducing processed food at one meal. The starting point matters less than the mindset behind it: you’re investing in resilience, not looking for a quick fix.
At Banner Peak Health, we help patients move beyond the reset mentality toward true metabolic wellness. If you’re ready to stop searching for the magic button and start building sustainable health, we’re here to guide that process.
What Is Hemoglobin A1C? How to Lower It Naturally
Think back to your school days.
At the end of each semester, you received a grade: a single number that reflected months of effort. That grade wasn’t your score on yesterday’s quiz. It integrated your homework, tests, attendance, midterm, and final exam into one indicator of how you performed over time.
Hemoglobin A1C works the same way for your metabolic health. But what is hemoglobin A1C?
This single blood test captures your average blood sugar control over the past 90 days. Unlike a semester grade that only affects your transcript, hemoglobin A1C is far more consequential. It reflects your risk for diabetes, heart disease, cancer, dementia, autoimmune conditions, and even depression.
Metabolic health influences almost every disease we face. That’s why knowing what hemoglobin A1C measures (and what you can do about it) matters so much.
What Is Hemoglobin A1C?
Hemoglobin is a large, iron-containing protein inside your red blood cells. Its job is to carry oxygen from your lungs throughout your body. Each red blood cell lives for approximately 90 days before being broken down and recycled.
Hemoglobin is made of four protein subunits, and two of these can irreversibly bind glucose. As glucose floats through your bloodstream, some of it attaches permanently to hemoglobin molecules. The higher your blood sugar runs, the more glucose binds.
Hemoglobin A1C measures the percentage of your hemoglobin that has glucose attached. A reading of 5% means 5% of your hemoglobin’s binding sites have glucose bound to them; a reading of 7% means 7% are bound. This percentage gives us a weighted average of your blood sugar over the lifespan of your red blood cells: about three months.
Hemoglobin A1C doesn’t measure a concentration in your blood at one moment. It measures the cumulative effect of your blood sugar over 90 days.
What Does Hemoglobin A1C Mean? Reading the Numbers
The American Diabetes Association defines the categories this way:
- Less than 5.7%: Normal
- 5.7% to 6.4%: Prediabetes
- Greater than 6.4%: Diabetes
“Normal” and “optimal” aren’t the same. The risk for insulin resistance and poor metabolic health climbs above 5.4%. If you’re aiming for the best metabolic health, keep that target in mind.
Why Blood Sugar Fluctuates: The Beach Ball Analogy
Many people imagine blood sugar as a simple pipeline: food goes in, sugar enters the bloodstream. But that’s not how it works.
Instead, picture a beach ball being pushed around by many Nerf guns firing from every direction. Each foam pellet nudges the ball a different way. Where the ball ends up depends on those competing forces.
Your blood sugar works the same way. At any instant, it’s being pushed and pulled by:
- What you ate and when you ate it
- Your stress and anxiety levels
- How much sleep you got
- Whether you exercised
- Your body’s hormone fluctuations
- How relaxed or tense you feel
These forces converge to produce your blood sugar reading at any given moment.
Hemoglobin A1C, by contrast, captures the cumulative result of all those pushes and pulls over 90 days. It measures where the beach ball has traveled on average rather than where it is right now.
How to Lower Your A1C Naturally: Two Steps
If hemoglobin A1C is your semester grade, think of a continuous glucose monitor (CGM) as your daily quiz scores. A CGM attaches to your body and measures glucose levels every five minutes, giving you real-time feedback on how your lifestyle choices affect your blood sugar.
But you don’t need a CGM to start improving your metabolic health.
Step One: Lower Hemoglobin A1C Naturally With Lifestyle Fundamentals
Start with the low-hanging fruit. Ironically, that often means reducing the foods in your diet that aren’t fruit:
- Cut ultra-processed foods and refined sugars. These spike blood sugar rapidly and offer little nutritional value.
- Increase physical activity. Exercise helps your muscles absorb glucose and improves insulin sensitivity.
- Reduce caloric intake if you carry excess fat mass. Visceral fat directly contributes to insulin resistance.
- Prioritize sleep. Poor sleep disrupts the hormones that regulate blood sugar.
- Acknowledge and address stress. Chronic stress elevates cortisol, which raises blood sugar.
These fundamentals form the foundation of metabolic health. Many people see meaningful improvement in their hemoglobin A1C by applying these principles over several months.
Step Two: Fine-Tune With Real-Time Feedback
If you want to go deeper, a continuous glucose monitor offers a granular view of your individual responses. You’ll learn what foods spike your blood sugar, how timing and food combinations matter, and how exercise and sleep affect your readings.
This is personalized medicine at its most practical. Rather than following generic advice, you learn what works for your body. At Banner Peak Health, we help patients with this kind of data-driven optimization.
Setting Realistic Expectations
Metabolic health unfolds over months and years, not days. You can only meaningfully recheck your hemoglobin A1C every three months, since that’s how long it takes your red blood cells to turn over and reflect your new patterns.
You won’t find a silver bullet for this. If you want to lower your A1C naturally, it requires an integrated approach: better nutrition, more movement, adequate sleep, and managed stress.
Today’s Takeaways
So what is hemoglobin A1C, really? It’s not a verdict. It’s information: a snapshot of where your metabolic health has been over the past three months.
If that number is higher than you’d like, start with the fundamentals in Step One. If you want more precision, consider working with a CGM to understand your body’s unique responses.
At Banner Peak Health, hemoglobin A1C is one of many tools we use to assess and optimize your health. We’re here to help you interpret your numbers and build a personalized plan to improve them.
Best Timing for a PSA Test: A Physician’s Guide for Middle-Aged Men
Back in 1979, a book called Don’t Buy a Car Made on Monday came out, using a humorous title to introduce the idea that what auto workers did over the weekend impacted their work quality on Monday. There was never hard data to support the assertion, but the idea became accepted folklore.
Let’s explore how the same principle may apply to PSA testing.
What the Prostate Does
The prostate secretes prostatic fluid, an integral part of the male reproductive system. This fluid provides the environment for semen to do its job: It serves as an energy source for spermatozoa, helps balance pH during intercourse, and creates the correct viscosity for reproduction.
Prostatic fluid contains a protein called prostate-specific antigen, or PSA. To know what to avoid before a PSA test, you first need to know how PSA gets into your bloodstream.
The Jelly Donut: Prostate Anatomy Explained
Think of the prostate as a prostatic fluid factory, made up of multiple coils of tiny tubes. The inside of each tube produces prostatic fluid, including PSA. These tubes are surrounded by the blood supply, with capillaries running alongside them.
The diagram below shows a cross-section of one of these tubes.

Think of each tiny tube as a miniature jelly donut. The interior jelly is the prostatic fluid (containing PSA), and the donut itself is the layer of cells that produce and contain it.
Anything that disturbs that little miniature donut and allows the jelly to leak out into the bloodstream will raise your PSA.
Why PSA Is Used for Cancer Screening
We use PSA to screen for prostate cancer because abnormal growth within the prostate disturbs the anatomy of those jelly donuts lined up inside it.
Cancer causes the donuts to leak their interior into the bloodstream, elevating PSA.
That’s why elevated PSA can signal a problem worth investigating.
The Problem: PSA Is Not Specific
Any single PSA that comes back abnormally elevated is a false positive 70–80% of the time.
Why so many false positives? Because there are many ways to disturb that jelly donut other than cancer.
What Can Disturb the Prostate (and Raise Your PSA)
Benign Prostatic Hypertrophy (BPH)
As men age, the prostate enlarges. This age-related growth is called benign prostatic hypertrophy. As everything expands and compresses, the jelly donuts become more prone to leaking.
This growth isn’t dangerous, just the normal wear and tear of aging, but your PSA can rise as a result.
Inflammation
If there’s inflammation in the prostate, whether from a bacterial infection or other causes, it creates disturbance in the jelly donut structure. Inflammation makes the junctions between cells more porous, and the jelly (PSA) leaks out.
This is called prostatitis, and it’ll elevate your PSA.
Trauma
Direct trauma to the prostate, whether from medical procedures in that area or from injury, can disturb the anatomy and cause PSA to enter the bloodstream.
Pressure From Cycling
Given the anatomy of sitting on a bicycle, particularly a road bicycle, force is applied to the perineal area. Over a number of hours, this external pressure from the bike seat transmits to the prostate, disturbing those jelly donuts.
Literature documents that a bike ride of several hours can cause a measurable elevation in PSA. So, how long do you need to avoid exercise before a PSA test? At a minimum, 48 hours after any extended cycling.
Sexual Activity
Ejaculation creates leakiness within the prostate’s epithelial cells and basement membrane. The process of secreting and ejaculating prostatic fluid disturbs the jelly donut structure, causing PSA to rise and enter the bloodstream.
How long before a PSA test should you not ejaculate? The same rule applies: at least 48 hours.
What to Avoid Before a PSA Test
For the most accurate PSA result, you need to be at least 48 hours removed from:
- Extended bike riding (especially road cycling)
- Sexual activity
If you have an ongoing prostatitis or infection in the genitourinary tract, you don’t get your PSA tested. Wait until the infection has resolved.
General Principles About PSA Testing
Because false positives outnumber true positives by a three-to-one or four-to-one ratio, the first thing to do when you see an abnormal PSA is repeat it.
Before you freak out, pursue further workup, or move to more sophisticated blood testing, anatomical imaging, or urine testing, push the pause button. Think through all the causes for false positives, make sure none of them apply, and then repeat the test.
I learned this adage in medical school: “A single abnormal test does not a disease make.”
When confronted with an elevated PSA, both the doctor and the patient become alarmed and want to move to the next steps immediately. Resist that urge. A careful, repeated test under the right conditions is the appropriate first response.
Today’s Takeaways
Who gets tested for PSA? Middle-aged men. If you’re too young, you don’t get tested. Too old, you don’t get tested.
And what do a lot of middle-aged guys do on the weekends? They go on long bike rides and have sex.
That artificially elevates their PSA on Monday.
Think about what to avoid before your PSA test: no cycling and no sexual activity for at least 48 hours beforehand. And if you do get an elevated result, don’t panic. Repeat the test under optimal conditions before pursuing further workup.
At Banner Peak Health, we take the time to think through the nuances of testing like this. A thoughtful approach to PSA screening can save you from unnecessary anxiety and invasive follow-up procedures.
How Long Should You Cold Plunge? A Physician’s Advice
Everyone wants to know the recipe: How long should you cold plunge? How cold should the water be? How many times per week?
The recommended protocol is 10–15 minutes in water between 50 and 59 degrees Fahrenheit, two to three times per week.
But understanding how cold water immersion works, and how to do it safely, requires a deeper look at what happens in your body during those minutes in icy water.
How Cold Water Immersion Works
Cold water immersion triggers two distinct mechanisms in your autonomic nervous system.
First, we have what’s called the diving reflex. Receptors in the skin of your face and upper body trigger your parasympathetic nervous system to respond when you’re fully immersed in cold water. This ancient reflex helped our ancestors survive underwater.
Second, the initial shock of cold water creates a surge of sympathetic discharge. Your body responds with peripheral vasoconstriction, increased heart rate, and elevated blood pressure. Then, your body tries to compensate by triggering increased parasympathetic tone.
This back-and-forth between sympathetic activation and parasympathetic compensation is where cold plunging becomes what I call “parasympathetic rehab” or “homeostasis training.”
Rethinking the Autonomic Nervous System
For years, I’ve explained the autonomic nervous system using a teeter-totter metaphor: the sympathetic nervous system (fight or flight) on one side, the parasympathetic nervous system (rest and digest) on the other, and balance achieved in the middle.
But that metaphor has a flaw. It suggests equal symmetry on each side, as if both systems play equivalent roles in our health.
They don’t.
A better metaphor is a sailboat in stormy seas.
The sympathetic nervous system is the sail and mast. It propels you forward, but it’s also a toppling force. In a strong wind, the sail wants to knock the boat over. Sympathetic overload is associated with disease.
The parasympathetic nervous system is the weighted keel below the waterline. It anchors the boat and keeps it upright. Parasympathetic strength is associated with resilience to disease and the ability to maintain homeostasis.
This ties into aging and longevity. Aging is about homeostasis: our ability to rebalance after the inevitable buffeting of life.
As we age, we don’t right our sailboat as well. The parasympathetic nervous system degrades. Heart rate variability (HRV), our best real-time measure of the balance between sympathetic and parasympathetic tone, declines with age.
Keeping the sailboat upright allows us to age more successfully.
Cold water immersion strengthens your weighted keel. It trains your parasympathetic nervous system to respond more effectively to stress.
The Well-Supported Benefits
Cold water immersion has advantages across several areas, and the literature supports these benefits well.
Sports Recovery
Studies show a reduction in delayed onset muscle soreness (DOMS). Cold water immersion has demonstrated benefits in muscle performance during jumping and sprinting, as well as reduced markers of muscle damage in the blood.
Mental Health and Sleep
Cold water can improve feelings of stress and negative emotions. It can help with relaxation and sleep quality, which makes sense given our discussion about sympathetic and parasympathetic balance.
Metabolic Health
Cold water immersion can increase the energy your body uses, which may help with metabolism.
A small percentage of our total fat is brown fat. Unlike white fat, brown fat burns calories to generate heat. Cold water immersion activates these fat cells, which can increase your basal metabolic rate. Evidence suggests that overall metabolic health improves with cold water immersion: lower blood sugar, better insulin sensitivity.
Cold Plunging: The Dangers You Need to Know
Rapid sympathetic discharge followed by compensatory parasympathetic response can be dangerous. This is why understanding how long and how to cold plunge is necessary for safety.
Cold Shock
Cold shock occurs when your body is immersed in water below 59 degrees Fahrenheit. Anyone who has jumped into a cold lake has probably experienced this. It’s an involuntary set of reactions that can last from a few seconds to about a minute, peaking around 30 seconds.
During that minute, you gasp involuntarily. Your breathing rate increases — hyperventilation. Your heart rate shoots up rapidly. Blood pressure surges. Peripheral vasoconstriction occurs.
If you’re immersed underwater, it’s a real drowning risk. You involuntarily open your mouth. You could aspirate, or even drown.
If you have any risk factors for cardiac arrhythmia, this sudden buffeting by the sympathetic surge and parasympathetic compensation creates risk for dangerous heart rhythms.
As a backpacker, I’m acutely aware that at elevation (6,000–10,000 feet), the hypoxia in the air accelerates all this and compounds the potential risk of cold shock.
One of my daughter’s classmates died while swimming in a mountain lake. He was college-aged and very healthy. It was probably a cold shock reaction.
When I go backpacking with my kids and they want to swim in a mountain lake, I tell them to stay parallel to the shore and not try to swim across the lake. People underestimate the risks of cold water at elevation.
Who Shouldn’t Cold Plunge
So, how long should you cold plunge? For people with the following conditions, zero minutes and zero seconds:
- Heart disease or any cardiac problems
- Uncontrolled blood pressure
- Raynaud’s disease
- Asthma
- Neuropathy
- Pregnancy
- Recent surgery
Nobody should practice cold-water immersion alone in open water, regardless of health. Have others nearby.
How to Start Safely
When beginning cold water immersion, don’t start by instantly putting your head under the water. For the first minute, keep your head above the water.
Start with just one to three minutes, two to three times per week.
You’ll adapt to cold water immersion over time. Like anything, build up gradually. Over weeks and months, you can work toward the 10–15 minutes recommended in the literature. If at any point you experience chest discomfort, lightheadedness, numbness, or dizziness, abort the mission.
Once you finish your cold water immersion, don’t run straight to a hot shower. That’ll give your system too much stimulation in the other direction.
Warm up more slowly. Towel yourself off, maybe have a hot beverage. Let your body regulate its temperature gradually.
Cold Plunging: A Potent Tool, Not a Silver Bullet
Cold water immersion can be a wonderful tool for enhancing parasympathetic tone and recovery after intense workouts, but don’t think of it as a standalone modality or silver bullet.
It’s an arrow in the quiver: one tool among many in a more robust parasympathetic rehab program that includes meditation, careful attention to breathing, Zone 2 cardio, and other lifestyle interventions.
At Banner Peak Health, we look for every possible mechanism to strengthen the parasympathetic nervous system and enhance our patients’ resilience. Cold water immersion, practiced safely and as part of a comprehensive approach, can be a valuable addition to that program.

How a Simple Nasal Spray May Help Prevent COVID and Colds
Getting COVID is never fun.
Last September, I attended a national physician conference and came home with an unwelcome souvenir: COVID. I developed a relatively mild case, but nonetheless, I wasn’t myself for at least a few weeks.
Fast-forward to the same conference in 2025. This time, I went armed with azelastine nasal spray, an over-the-counter antihistamine commonly used for allergies. I applied one spray in each nostril twice a day.
The meeting became what most would call a superspreader event: More than 20 of about 100 attendees caught COVID. But I dodged the bullet.
The Science: Blocking the Virus at the Gate
Azelastine isn’t new. It’s been used safely for decades to treat allergic rhinitis. What’s new is our understanding of how it might protect against respiratory viruses.
COVID and many other upper respiratory infections begin in the nose. The COVID virus binds to ACE-2 receptors on nasal cells — the same area azelastine coats when sprayed.
In laboratory and animal models, azelastine disrupts viral entry, reduces local inflammation, and even interferes with enzymes needed for viral replication. It seems to make the nasal environment less hospitable to infection.
The CONTAIN Trial: From Theory to Proof
In 2025, researchers at Saarland University Hospital published the CONTAIN trial in JAMA Internal Medicine.
Four hundred fifty healthy adults used either azelastine 0.1% or a placebo three times daily for 56 days. Participants self-tested twice weekly for COVID and were screened for other viral infections when symptomatic.
Results:
- COVID infection occurred in 2.2% of the azelastine group vs. 6.7% of the placebo group — a 69% reduction in risk.
- Colds caused by rhinovirus were also reduced (1.8% vs. 6.3%).
- Side effects were mild — mostly a brief bitter taste or a minor nose irritation.
Azelastine’s effect was localized, safe, and surprisingly broad, suggesting protection not only from COVID but also from everyday URIs.
Why This Matters
Vaccines and antivirals remain our strongest defenses against severe disease, but their ability to prevent infection wanes over time and with new variants. Azelastine adds another layer: a topical, low-cost, non-systemic option that can be started immediately and used intermittently — say, during travel, conferences, or cold-and-flu season.
Because azelastine is already FDA-approved for allergies, it’s accessible and familiar. Its mechanism is preventive, not curative. It’s a daily shield, not a rescue medication.
Sometimes, progress doesn’t require a new drug — just a new way of using an old one.
Today’s Takeaways
- Azelastine nasal spray, taken two to three times daily, reduced COVID risk by ~70% in a clinical trial.
- It may also lower rates of other respiratory infections.
- Side effects are mild and local.
- Consider using it during high-exposure settings such as travel, gatherings, or conferences.
- Larger studies are underway, but early evidence is promising.
- Available without a prescription.
At Banner Peak Health, we continue to explore evidence-based, practical tools for optimizing resilience. Sometimes, the simplest interventions, like a nasal spray, can make the biggest difference.